
The Sentinel Surveillance Network identified one case of influenza-like illness, which reaches the threshold that is applicable to the interepidemic season, according to the European Center for Disease Prevention and Control (ECDC) guidelines.
Regarding SARS-CoV-2 genomic surveillance, the Laboratoire national de santé analysed 221 specimens in week 31/2021 (from 404 total cases in the Grand Duchy of Luxembourg, 54,7%), including 180 non-targeted specimens (44,6%). This exceeds the minimum coverage (10%) but does not reach the minimum sample size (242) recommended by the ECDC.
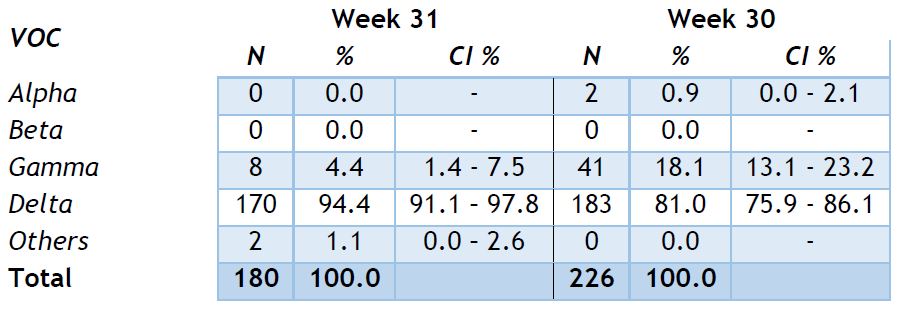
Community surveillance showed that Delta variant continues to be the dominant one in Luxembourg (94,4%), with low presence of the Gamma (4,4%) and other variants (1,1%).
In respect to target group surveillance, all cases analysed were identified as VOC cases and 16 post-vaccination breakthrough cases were identified as VOCs.

The Laboratoire national de santé, as National Reference Laboratory for Acute Respiratory Infections in Luxembourg, performs close surveillance on respiratory viruses, with a special focus on SARS-CoV-2. There are currently three active projects:
The Sentinel Surveillance Network. It provides a broad picture of respiratory diseases affecting the Luxembourgish population, based on its double monitoring system (syndromic and virological).
The National SARS-COV-2 Genomic Surveillance Program. It enables detailed observation of SARS-CoV-2 mutations and variants through time and space, and also monitoring specific groups of interest.
The COVVAC Serology Project. It assesses the post-vaccination serological status in long-term care facilities and its evolution over time.
The ReViLux provides updates on the first two projects.
The Sentinel Surveillance Network aims at monitoring the circulating respiratory viruses, including SARS-CoV-2, and hence underpin public health actions. Following the World Health Organization (WHO) and European Centre for Disease Prevention and Control (ECDC) guidance, it focuses on cases of acute respiratory infection (ARI) and influenza-like illness (ILI).
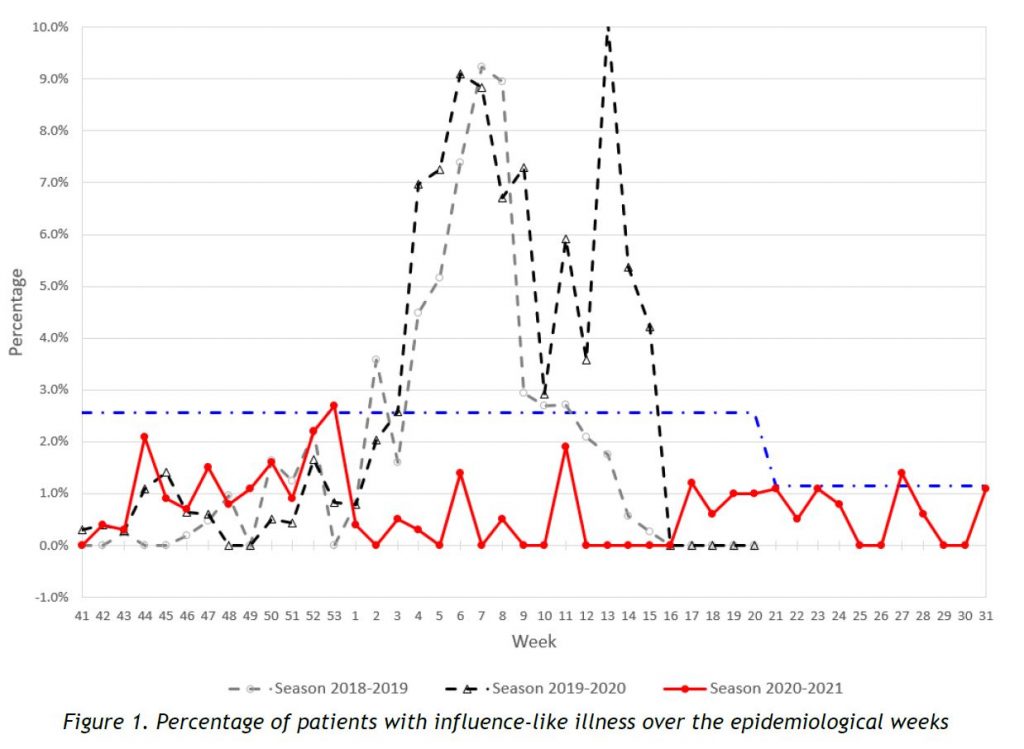
Results of syndromic surveillance during week 31 (02 August 2021 – 08 August 2021) are displayed in Table 1 and the history of ILI consultations since the 2018-2019 season is shown in Figure 1. Only 1 case of ILI was identified, but as the number of consultations dropped to 87, the proportion of ILI cases in week 31 exceeds the threshold for the interepidemic season (1,14%) according to the ECDC. A close look will be kept at the evolution of ILI cases next week.
Regarding the virological surveillance, no data is available for week 31.

The National Reference Laboratory for Acute Respiratory Infections at LNS receives SARS-CoV-2 -positive samples for (nasopharyngeal or oropharyngeal swabs analysed by RT-PCR) from the national network of laboratories and proceeds as follows:
Sequencing all specimens from hospitalized cases.
Sequencing all specimens from reinfection and post-vaccination cases.
Sequencing all specimens from cluster cases.
Sequencing a sample of community cases.
The sample of community cases is a selection from all cases to detect emerging SARS-CoV-2 variants and early increases in their incidence and transmission within the community in Luxembourg. This sample is selected according to the ECDC guidelines.
In week 31, 404 new cases were registered in Luxembourg; hence, the minimum sample size required to detect a 2.5% incidence is estimated to be 242 specimens (59,9%). The number of non-targeted specimens from Luxembourgish residents, successfully sequenced this week was 180 (44,6%), which exceeds the minimum coverage (10%) but does not reach the minimum sample size (242) recommended by ECDC.
The LNS shares its sequencing results with GISAID EpiCov database (www.gisaid.org) periodically. SARS-CoV-2 lineages (variants) have been assigned based on Rambaut et al. using Phylogenetic Assignment of Named Global Outbreak LINeages (pangolin) software (v3.1.10, pangoLEARN 2021-07-28). The ReViLux continues to use the Pango nomenclature, in addition to the WHO nomenclature, to allow easier visualization of links between any evolving variants and their ancestor (https://cov-lineages.org). See nomenclature equivalences in Annex 1.
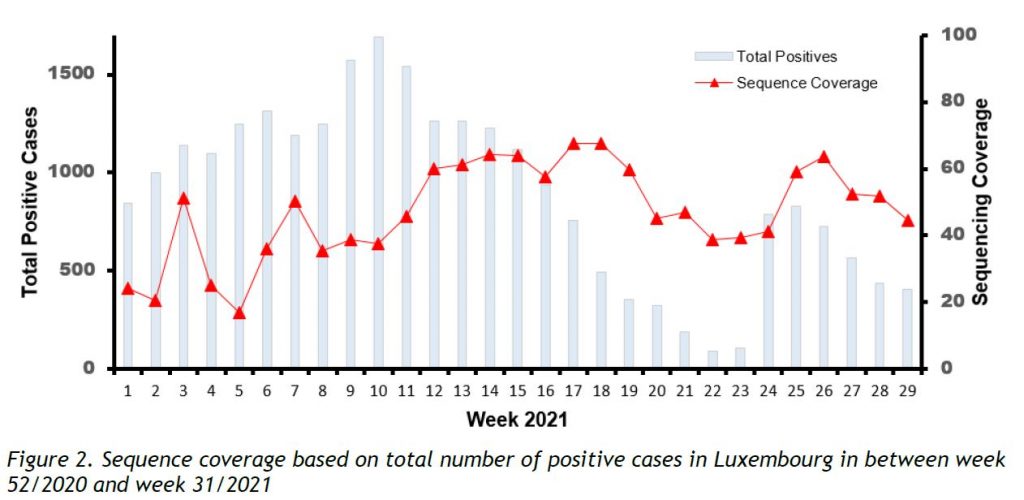
Last week, the microbial genomics platform at the LNS sequenced 252 specimens, with 248 having been collected in week 31/2021. Among the latter, 61 specimens were reported to be part of a cluster or non-residents. The number of non-targeted specimens from Luxembourgish residents successfully sequenced this week was 180 (44,6% coverage of 404 total cases) (see coverage trend in Figure 2).
The evolution of variants over the weeks is shown in Figure 3.
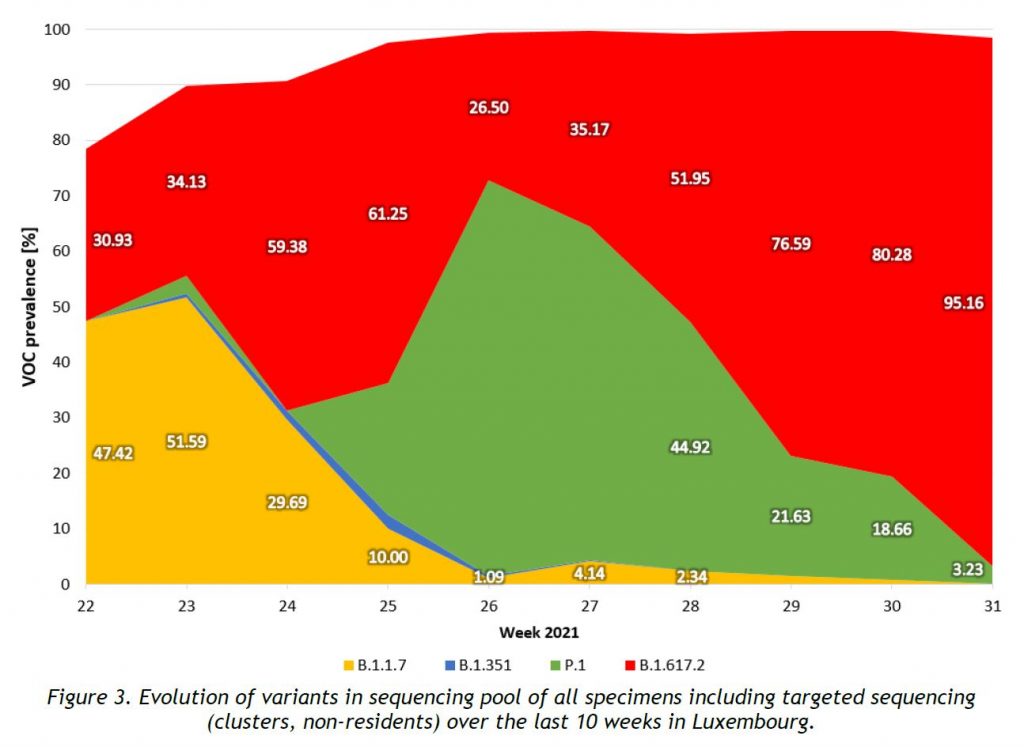
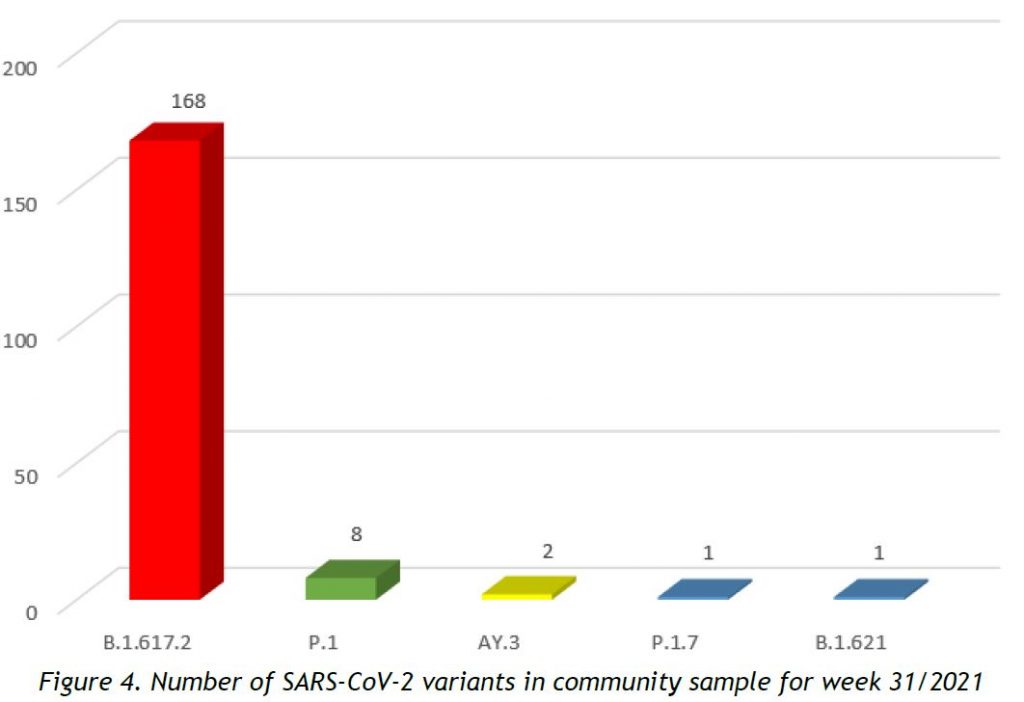
In week 31/2021, 5 circulating SARS-CoV-2 variants were detected within our population sequencing pool, after removal of cluster specimens, and excluding specimens collected from non-residents, as shown in Figure 4. The most prevalent lineages are displayed in Table 2 and information about the lineages is provided in Annex 2.
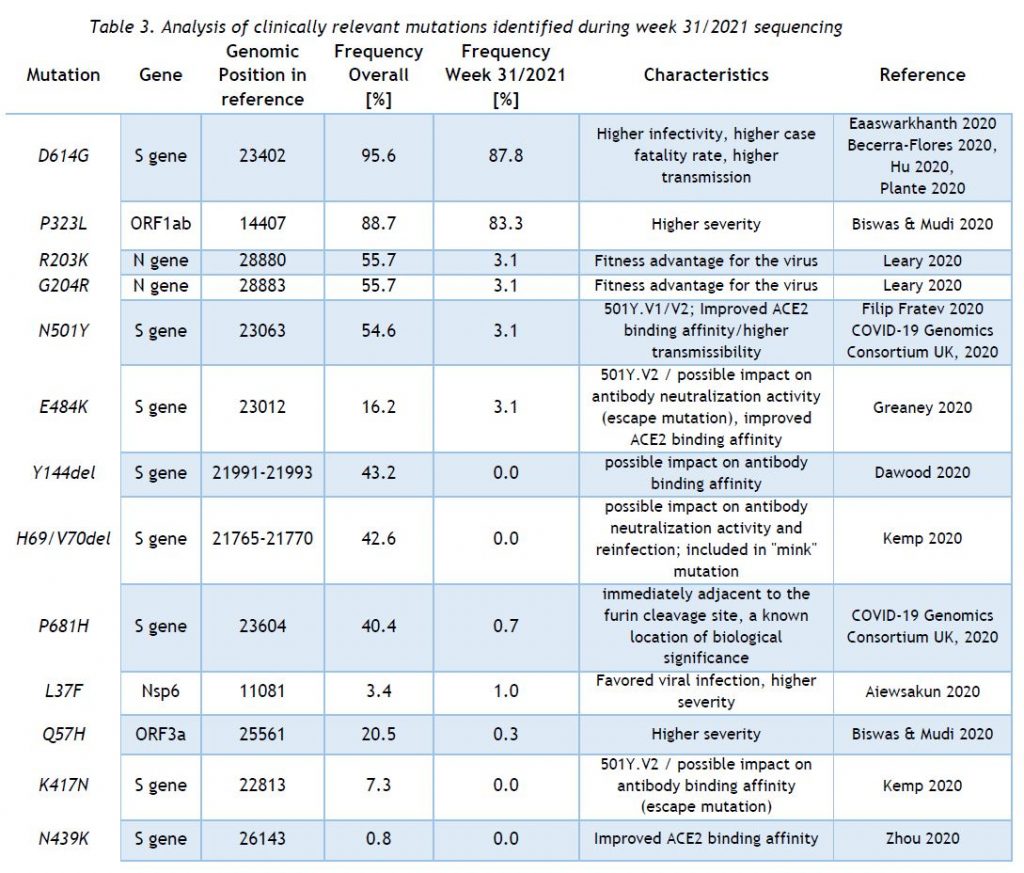
In addition to the surveillance of SARS-CoV-2 variants by whole genome sequencing, the LNS monitors the occurrence of SARS-CoV-2 mutations assumed to have a clinical and epidemiological relevance. Currently, 13 mutations are being observed, and this list is updated continually.
Table 3 provides the overall frequencies of these mutations, detected in the lineage-assignable genome sequences, analyzed since 1 Sep 2020 (N=16679), as well as the frequencies in week 31/2021.
COVID-19 Data Portal – accelerating scientific research through data. (2021). Retrieved 2 August 2021, from https://www.covid19dataportal.org/sequences
European Centre for Disease Prevention and Control. Guidance for representative and targeted genomic SARS-CoV-2 monitoring – 3 May 2021. ECDC : Stockholm ; 2021
Genomic sequencing of SARS-CoV-2: a guide to implementation for maximum impact on public health. Geneva: World Health Organization; 2021.
GitHub – cov-lineages/pangolin: Software package for assigning SARS-CoV-2 genome sequences to global lineages. (2021). Retrieved 2 August 2021, from https://github.com/cov-lineages/pangolin
Hadfield J., Megill C., Bell S., Huddleston J., Potter B., Callender C. et al. (2018). Nextstrain: real-time tracking of pathogen evolution. Bioinformatics, 34(23), 4121-4123. doi: 10.1093/bioinformatics/bty407
Rambaut A., Holmes E., O’Toole Á., Hill V., McCrone J., Ruis C. et al. (2020). A dynamic nomenclature proposal for SARS-CoV-2 lineages to assist genomic epidemiology. Nature Microbiology, 5(11), 1403-1407. doi: 10.1038/s41564-020-0770-5
The ReViLux continues to use the (Pango) system to allow easier visualisation of links between any evolving variants and their ancestor. Equivalence for most frequently used VOC nomenclatures are shown in Table A1 (adapted from WHO).
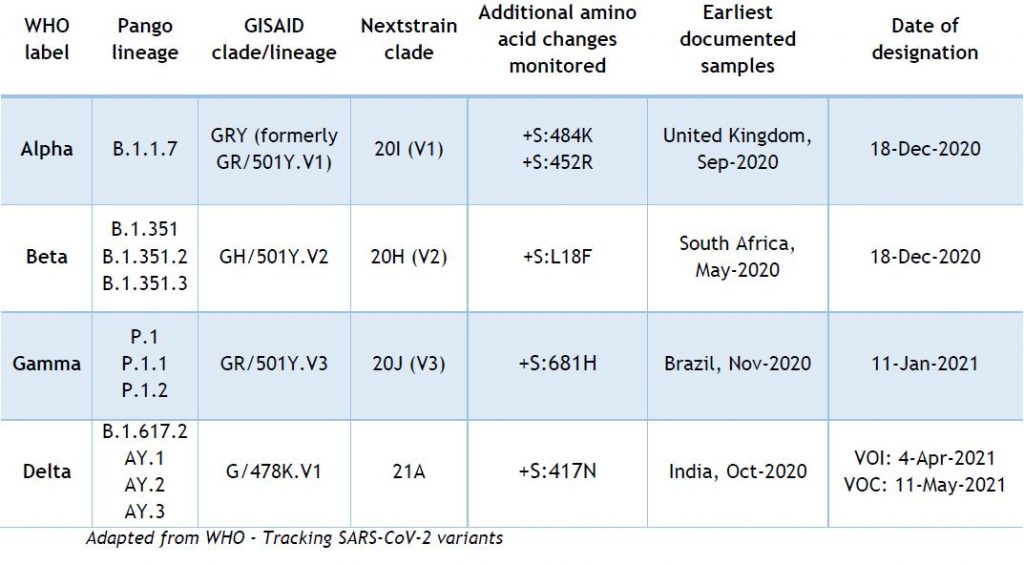
Lineage B.1.1.7 is characterized by several spike protein mutations, including N501Y, H69/V70del and P861H. The variant seems to have a considerable epidemiological impact, as it has a higher transmissibility rate.
Lineage B.1.351 holds numerous spike protein mutations, of which three are located in the receptor binding domain (K417N, E484K and N501Y), and are therefore relevant for antibody binding. As for B.1.1.7, a higher transmissibility rate and viral loads seem to be associated with this variant. Due to the K417N and E484K mutations, an impact on vaccination efficacy and possibility of reinfection is subject to scientific investigation.
Lineage P.1 (descendent of B.1.1.28), initially found in the Amazon region, has a similar mutation profile as the South African variant, including E484K and N501Y. Concerns are, as for the South African variant, higher transmissibility and a decreased protection by neutralizing antibodies.
Lineage B.1.525 carries several mutations of biological significance, including E484K, Q677H and F888L. It does not carry N501Y, but a set of deletions similar to the B.1.1.7 variant.
Lineage B.1.617 is a variant first detected in India and was designated “Under Investigation” on 1st April 2021 by Public Health England. It contains a number of spike mutations associated with antigenic escape or found in other variants of concern, including L452R, E484Q and P681R. Subtype B.1.617.2 does not carry S:E484Q and seems to be more transmissible than B.1.1.7 (increasing confidence). Neutralization studies show reductions in cross-neutralizing activity between B.1.1.7 and B.1.351.